|
Bladder cancer is the 4th most common cancer amongst men and 8th most common in women. Most cases are related to smoking or industrial exposure to certain carcinogenic agents. The commonest symptom of this cancer is passage of blood in the urine which is either visible (macroscopic) or invisible (microscopic). Some patients may simply experience increased urinary frequency. Diagnosis of bladder cancer involves combination of diagnostic tests including urine examination, scans and diagnostic telescopic examination (Cystoscopy) of the bladder using a flexible telescope. Once diagnosis has been established patient has to undergo removal of the tumour by a procedure called transurethral resection. Traditionally this has been carried out using white light. As tumours vary in size some of these are not clearly visible and hence missed at these examinations. Studies have proved that in almost 25% patients some tumours are missed using traditional methods of bladder assessment. Hence patients need repeat procedures for removal of these missed tumours.
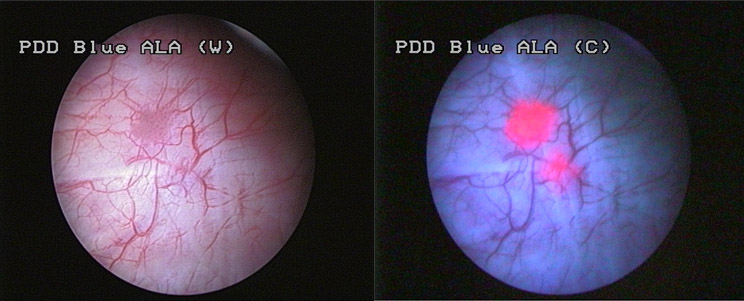
To improve the diagnostic accuracy of cystoscopy a special dye (HEXVIX) is instilled into the bladder an hour before bladder examination. This dye is selectively taken up by the cancer cells. When such cells are exposed to a special blue light tumours give out fluorescence which can be easily seen. This allows easy identification of all size tumours thus minimising risk of missing any tumours. Following pictures compare the appearance with standard and blue light cystoscopy.
Once the diagnosis of bladder cancer has been made treatment of the bladder cancer depends upon the depth and extent of bladder involvement, and nature of the cancer cells. Those tumours which remain confined to the lining can be removed through the telescope completely. However, additional treatment is usually given to reduce the risk of recurrence of the tumours. Such a treatment is administered via a catheter in to the bladder either as single treatment or multiple treatments on weekly basis for 06 weeks or longer. In cases where the tumours have grown deep into the wall of the bladder, curative treatment would involve total removal of the bladder and prostate in males and bladder, uterus and ovaries in females. This is called radical cystectomy in males and anterior exenteration in females.
Removal of the bladder for cancer is one of the most major operations in urology involving removal of the bladder and prostate in males and bladder with uterus and ovaries in females. After bladder removal various types of procedures are performed to substitute for bladder function. These include: 1) Simple conduit (Ileal Conduit) requiring wearing of bag for collection of urine. 2) Reservoirs made from bowel needing intermittent passage of catheters by the patient (Continent Urinary Diversion) 3) Reconstruction of a new bladder from bowel at the site of the original bladder (Orthotopic Badder). The choice is made depending on individual’s disease status, physical fitness, kidney function and ability and willingness to perform self catheterisation if required.
Traditionally removal of the bladder or radical cystectomy has been performed by open surgery. This entails longer incisions, excessive blood loss, slower recovery and poor cosmetic result. Recently new technologies including laparoscopy (Keyhole) and robotics have been introduced to minimise the disadvantages of the open operation. Robotics is currently the most advanced minimally invasive technology employed to carry out this procedure. It allows the surgeon to do a more precise job with minimal blood loss through small incisions which allows quicker recovery from surgery and better cosmetic result. The main features which render robotics superior to standard laparoscopy (Key Hole Surgery) are as follows:
These unique features translate into following advantages for the patient.
We have already performed more than 40 operations with excellent results.
|
|||||
|